
Cutaneous Fungal Infections in Children: A Common Concern and Effective Treatments
May 28, 2023
Cutaneous fungal infections, also known as dermatophytoses or ringworm infections, are a prevalent concern among children worldwide. These infections are caused by various fungi that thrive on the surface of the skin, hair, and nails. The warm and moist environments commonly found in children’s living spaces, such as schools and daycare centers, contribute to the spread of these infections. Fortunately, with prompt recognition, proper management, and effective treatments, cutaneous fungal infections can be easily controlled and cured in children.
Types of Cutaneous Fungal Infections:
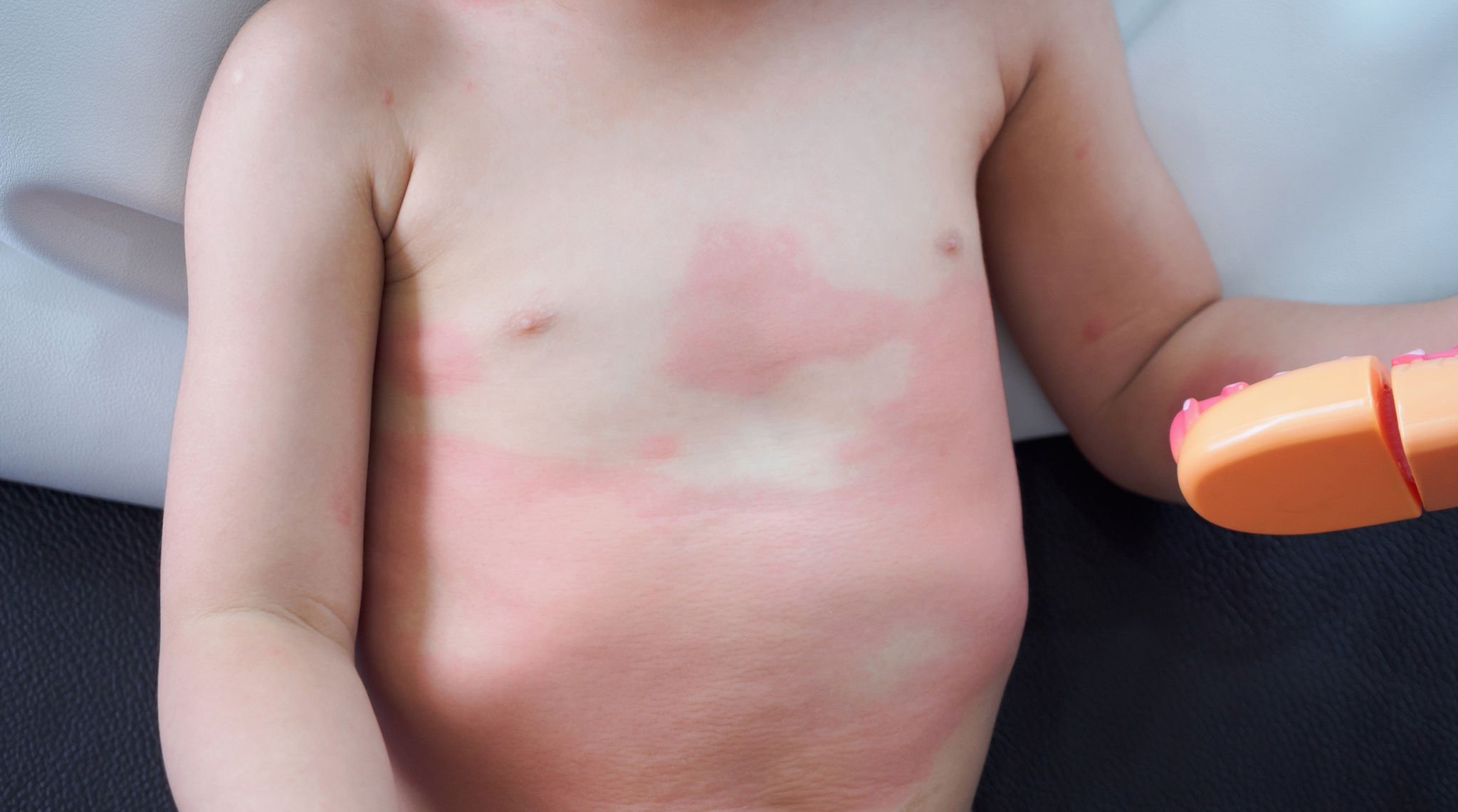
The most common types of cutaneous fungal infections in children include tinea corporis (ringworm of the body), tinea capitis (ringworm of the scalp), tinea pedis (athlete’s foot), tinea cruris (jock itch), and tinea unguium (nail infections). Each type manifests differently and requires specific approaches for diagnosis and treatment.
Symptoms and Diagnosis:
Cutaneous fungal infections in children present with characteristic symptoms. Tinea corporis appears as red, scaly, and itchy circular rashes, often with a clear center. Tinea capitis causes hair loss, scaling, and patches of broken hair on the scalp. Tinea pedis and tinea cruris manifest as itchy, red, and sometimes blistered rashes between the toes or in the groin area, respectively. Tinea unguium affects the nails, causing thickening, discoloration, and brittleness.
To diagnose cutaneous fungal infections, healthcare providers often perform a physical examination and may obtain skin scrapings or nail clippings for laboratory testing. Microscopic examination or fungal cultures can confirm the presence of fungi and identify the specific species involved.
Treatment Options:
Treating cutaneous fungal infections in children typically involves antifungal medications, either topical or oral, depending on the severity and location of the infection. Topical antifungal creams, ointments, or powders are usually prescribed for mild to moderate infections. These medications need to be applied to the affected area and its surrounding skin for a specific duration as directed by the healthcare provider.
In cases of severe or widespread infections, oral antifungal medications may be necessary to eliminate the infection entirely. It is crucial to complete the full course of treatment, even if the symptoms improve, to prevent the recurrence of the infection.
Prevention Strategies:
Preventing the occurrence and spread of cutaneous fungal infections in children requires certain precautions. These include:
- Maintaining good personal hygiene: Encouraging children to wash their hands regularly and bathe with mild soap can help reduce the risk of infection.
- Keeping the skin dry: Moisture can contribute to fungal growth, so it is important to ensure that children’s skin, especially in areas prone to sweating, remains dry.
- Avoid sharing personal items: Children should be advised not to share towels, clothing, hairbrushes, combs, or other personal items that may harbor fungi.
- Promoting awareness in schools and daycare centers: Educating children, parents, and teachers about the signs, symptoms, and preventive measures of cutaneous fungal infections can play a significant role in minimizing their spread.
Conclusion:
Cutaneous fungal infections in children are a common occurrence, often attributed to their active lifestyles and close proximity in communal environments. However, with early detection, appropriate treatment, and preventive measures, these infections can be effectively managed. Parents and caregivers should be vigilant in recognizing the symptoms and seeking prompt medical attention when necessary. By implementing preventive strategies and maintaining good hygiene practices, we can significantly reduce the incidence and impact of cutaneous fungal infections in children, ensuring their well-being and healthy development.
